By Aubrey Wursten
In a conclusion that has become predictable, a recent study by peer-reviewed journal Health Affairs found that when compared to all states, Alaska once again had the highest health spending per capita. Alaska also suffered one of the highest rates of increase in these costs. Additionally, the authors determined that Medicaid expansion was actually associated with growth in costs, and they discovered that this higher spending did not necessarily even correlate with improved outcomes in care.
Cost Comparisons Across State
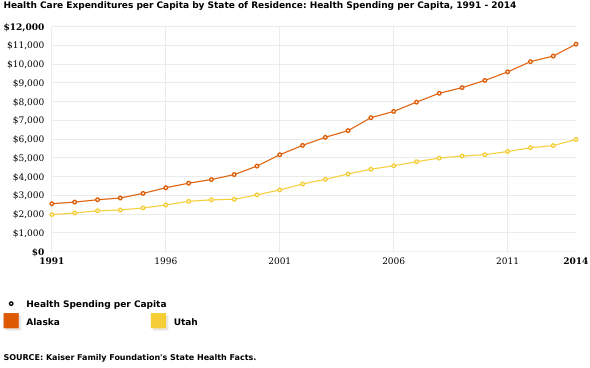
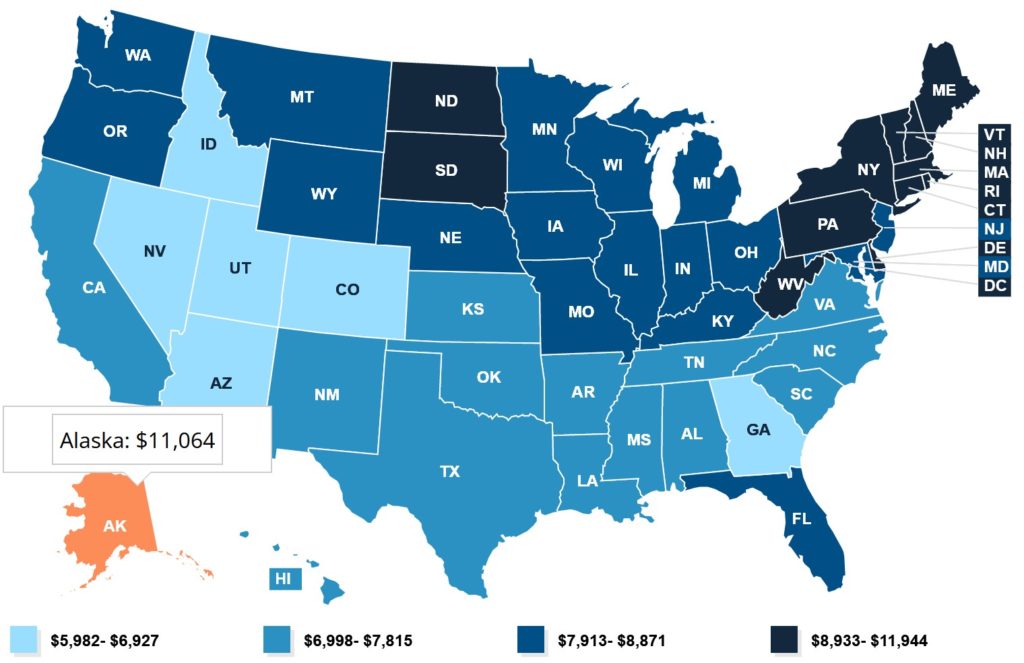
In 2014, the last year for which the government’s State Health Expenditure Accounts (SHEAs) offered comprehensive estimates, Alaska health spending per person reached $11,064. This exceeded the expenditures in any other state, and it was nearly double the $5,982 price tag in Utah, the state with the lowest costs per capita.
Although SHEA numbers were not available after 2014, the regression methods used by Health Affairs estimated a cost of $14,500 per capita in 2019 in Alaska, now exactly double Utah’s cost, estimated at $7,250. Adjusting for inflation, this showed that Alaska likely suffered an increase of 3.6% from 2013, far above the lowest state hike of 1%, estimated for Washington, D.C.
Correlation With Medicaid Expansion
Health Affairs researched the effect of several factors on health care costs, one of which was Medicaid expansion. Because the 2014 Medicaid expansion under the Affordable Care Act (ACA) coincided with the end of SHEA data collection, it was impossible to use those data to precisely gauge the impact that the expansion had on expenditures, but by utilizing primary data and regression methods, Health Affairs found that increases were associated with expansions. The research determined that “Medicaid-specific standardized spending” per capita from 2013 to 2019 for early Medicaid expansion states was 4.2%, compared to 2.6% in nonexpansion states.
Is Higher Spending Associated With Improved Patient Outcomes?
When adjusted for inflation, Health Affairs found that national health spending per capita doubled between 2000 and 2020, and it increased as a share of the economy from 13.3% to 19.7%. But as Health Affairs notes, “Even as health care spending becomes an increasingly dominant portion of the US economy, health outcomes are falling short of national expectations for what this spending should deliver.”
Despite the jump in health care spending, life expectancy in the United States has recently begun to decrease for the first time in nearly a century. As noted, Alaska has the highest costs in the nation, yet as of 2020, it has a life expectancy of 76.6 years, compared to Hawaii’s high of 80.7 years.
Real Solutions
So, if higher costs are not the solution to poor health outcomes, and more regulations are not the solution to high costs, what measures could contribute to better results in both costs and health in Alaska?
Certificate of need (CON) laws, to which Alaska is subject, prevent new health care companies from opening and bar existing ones from expanding. These barriers-to-entry consistently lead to less access to care and to higher prices for the care that remains available. States with CON laws tend to have fewer hospital beds and other equipment, and the lack of competition allows current practices to charge higher prices than they could otherwise expect. Eliminating CON legislation, as 15 other states have already done, would be an effective step to improve health care in the state.
Another measure that has proven especially effective in lowering costs is easing restrictions on telehealth. Alaska has a unique need to access health services by internet, as its residents are often living far from a brick-and-mortar clinic. Alaska Policy Forum affirms that “All Alaskans, including those in rural areas with limited providers and facilities, the homebound elderly, and the immunocompromised, should have timely access to the health care provider of their choosing.”
Just as a patient suffering from strep throat has no need to check into an emergency room and pay the exorbitant related fee, a patient with a clearly visible (and contagious) eye infection has no need to step into a clinic. Many routine visits could be conducted online, saving the costs associated with in-house care, as well as increasing competition by expanding the pool of available doctors.
Finally, removing roadblocks to direct care practice offers another way for patients to control their own health care costs. Direct care allows patients and their chosen providers to work out a mutually beneficial payment arrangement that avoids the middleman of an insurance company for basic care. They can settle on an acceptable monthly fee, for which patients can expect as frequent access as they need to their provider. This results in more regular low-level and preventive care, which also leads to less frequent need for more expensive and invasive procedures.
Conclusion
Alaska has at its disposal several potential policies to increase health care access and decrease spending. The measures taken thus far involving more government intervention have failed by virtually every metric. Alaska legislators would do well to learn from past mistakes and focus on less intrusion, by taking steps to repeal CON, expand telehealth, and protect direct care practices.
Aubrey Wursten is APF’s Summer 2022 Policy Intern. She is currently studying at Brigham Young University-Idaho.