Dust off Alaska’s Statutes and Eliminate Them
Click here to open a printable PDF of the policy brief in a new tab.
Alaska has incredibly high health-care costs, and a recent report by a nationally respected healthcare economist demonstrates that our state’s certificate of need (CON) program is one of several reasons why.[1] Over the years, research from a variety of economists and antitrust lawyers have found that CON laws increase costs, limit accessibility, and discourage quality health care.[2] A simple solution in response is to repeal Alaska’s archaic CON program.
Alaska’s CON program requires potential health-care service providers to get permission from the state government before opening a new facility, expanding an existing facility, or purchasing new equipment, including additional hospital beds. The potential service provider must attempt to prove to state bureaucrats that the community needs the new or expanded facility, and existing service providers are solicited to testify against the would-be competitor’s application. The application and approval process is lengthy, expensive, and prohibits service providers from expanding patient options and from responding in real-time to community health needs, such as a pandemic.
Certificates of need were mandated by the federal government in 1974, in the hopes that they would slow down quickly inflating health-care costs, as well as improve accessibility and quality of health care.[3] By 1987, however, Congress repealed the mandate, as they found it did nothing to curb health-care costs, and in fact increased them. Today, 12 states have abolished their CON programs, and Alaska should follow suit.
By regulating new facilities and expansions, the state decreases competition and increases prices. According to the Federal Trade Commission, “[b]y interfering with the market forces that normally determine the supply of facilities and services, CON laws can suppress increases in supply and misallocate resources. They also shield incumbent health-care providers from competition from new entrants and innovations in health-care delivery, which means consumers lose these benefits.”[4] Additionally, the CON application process itself is a costly, lengthy endeavor and discourages would-be applicants from even beginning.
 To put it simply, eliminating Alaska’s CON program would result in more competition and lower consumer health-care prices. A study by the Mercatus Center found that repealing Alaska’s CON requirements would save $294 per capita annually on health-care costs and $129 per capita annually on physician spending.[5]
To put it simply, eliminating Alaska’s CON program would result in more competition and lower consumer health-care prices. A study by the Mercatus Center found that repealing Alaska’s CON requirements would save $294 per capita annually on health-care costs and $129 per capita annually on physician spending.[5]
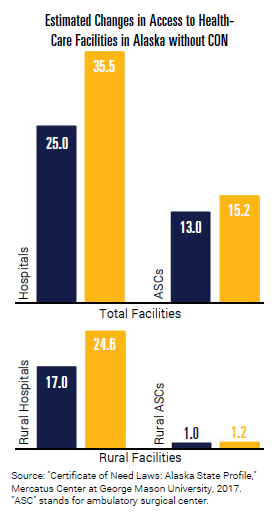
Research has also found that CON laws limit health-care accessibility.[6] In Alaska, CON laws particularly affect rural areas, leading to fewer rural hospitals and ambulatory surgical centers compared to states without any CON requirements. In fact, without CON requirements in Alaska, there could be nearly 25 hospitals in rural areas, rather than the current 17.[7]
In addition, CON laws were originally implemented to encourage quality health care. However, in practice, this has not been the case. Without CON requirements, overall quality ratings of Alaska hospitals would improve, heart attack and heart failure readmission rates would decrease, and deaths from post-surgery complications would decrease by an estimated 5.6 percent.[8] Opening up the market to competition incentivizes innovation and efficiency, leading to increased quality of care. Additionally, when there are multiple locations for a patient to receive care, patients are more able to “shop around” or switch providers when not receiving quality care. This encourages providers to increase quality and decrease prices.
In the spring of 2020, many states, including Alaska, temporarily suspended CON laws in response to COVID-19, so that hospitals could be more flexible in providing beds and care where needed.[9] To increase accessibility, quality care, and drive down high costs, Alaska should make this temporary suspension permanent and repeal all other components of its CON program as well. In the words of one author, repealing CON laws is one step in “try[ing] to raise the bar and not just flatten the curve” when it comes to health care.[10]
Endnotes
[1] Ippolito, Benedic, Controlling Health Care Costs in Alaska, Alaska Policy Forum, June 30, 2020, https://alaskapolicyforum.org/wp-content/uploads/2020-06-30-APF-Health-Care-Costs-in-AK.pdf.
[2] Competition in Healthcare and Certificates of Need: Before A Joint Session of The Health and Human Services Committee of the State Senate and The CON Special Committee of the State House of Representatives of the General Assembly of the State of Georgia, (2007) (testimony of Mark J. Botti), https://www.akleg.gov/basis/get_documents.asp?session=31&docid=23753.
[3] Accosta, Alexander, Alex M. Azar II, and Steven T. Mnuchin, “Reforming America’s Healthcare System Through Choice and Competition,” U.S. Department of Health and Human Services, 2019, https://www.hhs.gov/sites/default/files/Reforming-Americas-Healthcare-System-Through-Choice-and-Competition.pdf.
[4] Statement of the Federal Trade Commission to the Alaska Senate Committee on Health & Social Services on Certificate of Need Laws and SB 1, (2019) (testimony of Daniel Gilman), https://www.ftc.gov/policy/advocacy/advocacy-filings/2019/03/statement-federal-trade-commission-alaska-senate-committee.
[5] Stratmann, Thomas, Christopher Koopman, Matthew D. Mitchell, Matthew C. Baker, and Anne Philpot, “Certificate-Of-Need Laws: How CON Laws Affect Spending, Access, and Quality across the States,” Mercatus Center at George Mason University, August 29, 2017, https://www.mercatus.org/publications/certificate-need-laws-alaska.
[6] Stratmann, Thomas, and Christopher Koopman, “Entry Regulation and Rural Health Care: Certificate-of-Need Laws, Ambulatory Surgical Centers, and Community Hospitals,” Mercatus Center at George Mason University, February 18, 2016, https://www.mercatus.org/publications/regulation/entry-regulation-and-rural-health-care-certificate-need-laws-ambulatory.
[7] Stratmann, Thomas, Christopher Koopman, Matthew D. Mitchell, Matthew C. Baker, and Anne Philpot, “Certificate-Of-Need Laws: How CON Laws Affect Spending, Access, and Quality across the States,” Mercatus Center at George Mason University, August 29, 2017, https://www.mercatus.org/publications/certificate-need-laws-alaska.
[8] Ibid.
[9] “Covid-19 Disaster Order of Suspension No. 2: Amendment 3 to Appendix A,” Alaska Department of Health and Social Services, April 14, 2020, https://gov.alaska.gov/wp-content/uploads/sites/2/04.14.20-Order-of-Suspension-2-Appendix-A-Amendment-3.pdf.
[10] Mitchell, Matthew D., and Thomas Stratmann, “Commentary: Let’s fix the laws around hospital capacity before the next health crisis,” Chicago Tribune, May 6, 2020, https://www.chicagotribune.com/opinion/commentary/ct-opinion-hospital-regulations-certificate-of-need-coronavirus-20200506-ku4mrntsxre73m4vq5jczvt7yq-story.html.